© Please note: Rita Van Horn owns the copyright for the dissertation below. You may download and print one copy for educational purposes only. These pages may not be duplicated, distributed, redistributed or republished in any manner without express permission from the author.
Introduction
From the first day of clinical experience, the student and teacher
are working and learning together. In this learning process, a
relationship is being established between the student and the
teacher to facilitate learning. The clinical experience involves
learning to solve problems, practicing new skills, improving on
previous nursing skills, and applying information learned in the
classroom to what is being observed and practiced in the clinical
setting.
The first part of this chapter includes vignettes from nursing
students who have written about their experiences in the clinical
setting. The descriptions were taken from the first day of clinical
experience, the middle of the quarter, and the last day of the
clinical experience. The purpose of sharing these vignettes is
to capture the lived experience of the students as they problem
solve during the 9 weeks of the clinical experience. The middle
part of the chapter includes statements of reflections the students
made in their journals. Journal writing was a method incorporated
during the quarter to assist the student in problem solving and
in thinking reflectively. The statements made by the student are
presentations of the process of reflection. The last part of the
chapter describes the themes that emerged from the students' written
journals. Because clinical experience is a complex learning experience,
as evidenced in the shared themes, the reader will catch glimpses
of this complex process.
Clinical Setting
Students were divided into two groups, one group met on Wednesday
and the other group which met on Thursday. The clinical day started
at 2:30 p.m. in a conference room at the hospital which is located
about 6 miles from the college campus. From 2:30 p.m. to about
3:00 p.m. (pre-conference time) the students shared the care plans
they had written from information they had collected from the
chart the night before clinical experience. I usually posted the
assigned patients about 4:00 p.m. the previous evening. I would
arrive about 20 minutes before pre-conference to review the condition
of the patients and to verify that the patients were still in
the hospital. Because of decreased patient time in the hospital,
there was no guarantee the patient would still be there by clinical
time. If the student's patient had been discharged, I would assign
a new patient to the student. During the pre-conference time I
discussed with the students changes in the patient's condition,
skills needed to be preformed during the shift, and new assignments
that had arisen. I would also answer questions about the patients
that the students would have from the information that was gathered.
Most of the time the questions involved medications that could
not be found in the drug books or a procedure that the student
had never performed or perhaps never seen before. The first 2
weeks the students had only one patient. By the third week, this
increased to two patients for a 9-hour period.
After pre-conference the students would proceed to their assigned
area to review the chart, medication sheet, and kardex (a form
that had the patient's activities, procedures, intravenous solutions,
and laboratory tests ordered by the doctor), and to ascertain
what changes had arisen since they had last collected the data.
The student would introduce him or herself to the nurse in charge
of the patient and receive a short report about the condition
of the patient. Students would organize their time on a schedule
form based on the information just obtained.
The student would then go and introduce him or herself to the
patient. The rest of the evening would include patient-care activities
such as medications, treatments, and preparing the patient for
bed, assessment of the patient's condition, and charting the activities
and events that may have developed during the time the student
was there. The student also spent time conversing with the patient
and the family as well as collaborating with the nurse on problems
as they arose throughout the evening.
After pre-conference, I made rounds to the four areas (intensive
care unit, cardiac care unit, medical-surgical unit, and transitional
care unit) where the students were located. During the first part
of the shift, I reviewed the care plans and the schedule the student
had designed. I had the student give me a short report about the
condition of the clients and discuss any problems.
I spent the rest of the evening in problem-solving activities
such as what to do with an elevated blood pressure, observing
procedures, validating the medications that were to be given to
the patient by the student, physical assessment of the patient
with the student, collaborating with the nurses and doctors, and
reviewing the charting the student had written. The last activity
before post-conference was a review of the charts and the medication
records to make sure all activities were completed.
Post-conference was about 45 minutes to an hour based on the time
we arrived to the conference room. At the beginning of the quarter,
I allowed the students to write in their journal the last 15 minutes
of the time together. I discovered that the students ended up
spending more time talking together instead of writing so I changed
the writing activity to the middle part of the conference. Post-conference
also included time for the group members to review what they had
learned and what problems they had struggled with during the night.
I would spend about 10 to 15 minutes demonstrating a procedure
such as tracheostomy care. We ended at 11:30 p.m. Because post-conference
was late at night, students struggled to stay awake. I often wondered
how beneficial the time was because of the lateness of the hour.
I was concerned with the drive home since some students lived
30-60 miles away.
Clinical Experience
The First Day
At the beginning of lab, I was really scared and overwhelmed.
I felt a little lost in orientation which led to a lot of stress
and anxiety. As a result, I think we students got frustrated and
started to doubt ourselves. I know I did, at least. I did not
think I was going to make it. I have noticed that in the past
two quarters, I have been "scared" of my teachers. It
does ruin, or at least slows down my learning (Journal 107, p.
3).
Since I have clinical experiences on Wednesday and Thursday, I
had two beginnings. In both groups there was an aura of anxiety.
This is normal, but the students do not think so. I sometimes
feel like a mother bird nudging her children out of the nest.
It is a long way to the ground. The students are reluctant to
go out the door of the conference room to get started. I had to
lead the way.
The first 2 hours of the shift were busy for me. I was concerned
whether the students would page me when they needed assistance,
or would they work on their own trying to solve problems beyond
their scope of practice. For these two nights I was supervising
students over only two areas of the hospital. What a difference
that was for the students! Because of close proximity with each
other, I noticed the students were able to more easily collaborate
with each other. Carol made this statement in her journal indicating
the importance of being with other students. I am really thankful
for my classmates tonight. They did not get tired of my questions.
Their smiles and their explanations helped me to care for the
patients (Journal 107, p. 1). This did change in 2 weeks. The
students were placed into four different areas on three different
floors of the hospital increasing the distance for me to observe
and making collaboration with each other difficult.
I am very timid with my patients and have too small of vocabulary.
Somehow I need to build up my vocabulary and learn to communicate
with the patients (Journal 107, pp 1, 2). As an instructor I had
tried to assure the students that I would be available to assist
them when they paged me on a beeper and I would answer their questions
when they talked to me, I am so afraid that I will make medication
errors and this made me more nervous (Journal 103, p. 2). Students
had commented to me that they hoped they would get a good nurse
to talk with, one who would understand their feelings and answer
their questions, one who would not think their questions were
stupid.
After assessing my patient's breath sounds, the patient complained
of having trouble breathing especially after waking up. I know
patients complaining of shortness of breath need assistance very
soon. I put the head of the bed up and contacted the respiratory
therapist. I explained to him the problem. After he and I assessed
breath sounds and checked the oxygen saturation level, we put
her on oxygen. The problem was solved (Journal 102, p. 1).
Although some anxiety is normal, I looked for severe symptoms
which could lead a student to be nonfunctional and unable to think
in the problem-solving process. These first 2 nights the students
had their anxiety under control. By post-conference time, they
were smiling and stating they were feeling better.
It is the end of the shift and I made it. I was able to set some
of my fears aside and put my knowledge into use. I am realizing
that the clinical experience is one of learning experiences, and
tonight I had a really good experience and feel nursing can be
a very exhilarating career as well as rewarding, I think. I was
able to step out of myself and concentrate on the patient and
this was most helpful (Journal 102, p. 3).
There was a difference in the two groups (Wednesday and Thursday)
in regard to personality and responsiveness. Wednesday's group
was more talkative and asked more questions. In fact, Linda asked
many questions—often before I had time to finish explaining
information—that I wondered if this was evidence of her fear
and at the same time I was somewhat irritated. In spite of my
feelings about the multiple questions Linda asked, I found Linda
well-prepared for clinical experience. Thursday's group was quieter.
There was a difference in the journals of the Wednesday group
versus the Thursday group. The Wednesday group seemed to express
more statements of confusion and anxiety. This disparity may have
resulted because I explained the information differently to Thursday's
group in response to the questions the Wednesday Group asked.
I am amazed at the differences, but I realize that I must address
the groups according to their differences.
Problem solving was seen in different forms on the first day.
There were two incidences of shortness of breath exhibited by
the patients. The first incident is described above in Joan's
vignette (Journal 102). The second one occurred when I was assisting
Terry. In the second incident, there was a difference in my perception
and Terry's perception as to how the problem was solved and what
events had actually transpired. Terry mentioned only the shortness
of breath in her description in her journal, but there was chest
pain accompanying the shortness of breath that was more serious.
In evaluating the differences in both students' journals (Joan
and Terry), I believe the knowledge used in solving the problem
and the ability to assess the patient was a weakness in Terry.
Terry did not use her knowledge base and exhibited poor assessment
skills in gathering data in order to solve the problem. This is
of great concern to me because if a student is weak in an area
such as using their knowledge, that student may make an incorrect
decision that could harm the patient. This was averted because
I was there to guide the student in alleviating the shortness
of breath problem.
The Middle of the Quarter
By the middle of the quarter, students were gaining more confidence.
Rose describes her clinical day: I had a hectic day, but overall
this clinical experience by far was the most educational for me.
During my shift my patient had a hypoglycemic attack. Her blood
sugar was 168, and I had given Regular Insulin, which was ordered.
She did not eat very much for supper, and two hours later she
was diaphoretic. I had looked up the word diaphoresis in Taber's
[Medical] Dictionary before I had come to the hospital so I knew
what it was. I did a finger stick for glucose and the result was
38 mg/dl. The LVN [licence vocational nurse] told me to give her
juice with sugar STAT [right now] to get her blood glucose up.
About 20 minutes later another blood sugar test was performed
and the blood sugar was 63 mg/dl. I was told to give her more
juice with sugar. But the patient was very weak, lethargic, drowsy,
and still sweating. I was afraid she may aspirate. The LVN put
sugar under the tongue which would be absorbed faster through
the membranes. The LVN also notified the doctor—something
I could not do. The doctor changed the sliding scale. About 2200
[10:00 p.m.] her blood glucose was up to 90 mg/dl, but still she
was weak and lethargic. At least the blood sugar level was up.
I think that tonight I found out how I handle myself in a situation
like this hypoglycemic reaction. I felt that I was more independent
and was not anxious over her attack. Even though I was a little
unsure about what exactly to do when a hypoglycemic reaction occurs,
I handled the problem better than I thought I would be able to.
I feel that even though I had questions for the RN [registered
nurse] and LVN, they still gave me the independence and encouragement
to be able to react to a crisis. With each clinical experience
my confidence with patient care increases (Journal 115, pp. 7,
8).
Sometimes a mistake is made by a student. This mistake can be
due to poor problem solving or ineffective thinking. As an instructor,
I wonder if the student has learned from her or his mistakes.
In reading Marie's journal, I found where she reflected on a mistake
that was made during her time with the patient. She gave the reasons
for the mistake she had made and what she was going to do next
time. The statement from her journal was as follows: I needed
to have asked myself why things were going the way they were and
I should have asked the nurse a question regarding why the NG
[nasogastric tube] was clamped. Although the nurse was busy, I
know now that next time I am going to ask, "Why" for
everything and try to come up with a solution right away. Even
though the staff might have been busy, I should not have felt
that my lab instructor or even the staff was too busy to help
me solve the problem.
Well, I hate to think that it took a mistake to help me learn
something new. I felt that I was not communicating as I should
have with my nurse, CNA [certified nurse assistant] or maybe even
the patient (I could have asked her about her own care; she was
keeping me on track sometimes). Now I understand the nurses a
little more when they are having a busy night. But I also realized
that many mistakes are more apt to occur on a busy night. From
now on, I am "gonna" take as long as I need to analyze
things and learn how to work with others even through busy times
(Journal 112, pp. 7, 8).
Reading this journal made me realize the importance of journals
and the trust factor that is involved in the journal writing.
I had talked with the student about the mistake that had been
made, but I did not know the impact of the discussion until I
read the journal. It took a lot of trust on the student's part
to write the information, but I knew then that the student would
grow as a result of the experience. The student became very conscientious
in asking questions and problem solving.
A different attitude permeates this class, which is something
I have not felt before. When I corrected students care plans,
they thanked me for the help. I usually get no reply or a grumbling
complaint. Appreciation for help was also written into the journals.
Cindy had a very anxious day in that she felt that she was not
prepared for caring for her patients. Her comment to me in the
journal was as follows: Rita, thanks for being so calm and not
being impatient with me. It was just what I needed at the time
(Journal 117, p. 14). Reading this made me realize the enormous
influence the teacher has on students, especially when students
are stressed for whatever reason. This statement made by Cindy
also made me feel appreciated and willing to continue in my practice.
The End of Quarter
By the end of the quarter, students are usually bringing the nursing
process problem-solving steps together no matter how small the
problem. For my patient J. D., I had picked anxiety as a nursing
diagnosis which applied to him, but I think his problem was more
than anxiety. He was very confused and saying a lot of things
that did not make sense. I believe he needs some psychological
help. His problem was a concern about having a bowel movement.
He had one in the morning but he stated that he felt pains in
his stomach and had the urge to have a bowel movement. The problem
was not an urgent one, but if I did not try to solve or address
the problem, he would have become very agitated. After I had assessed
his symptoms, I checked his chart and kardex to see if there were
any PRN [whenever necessary] orders for enemas or laxative. I
talked with the nurse. He and I did a rectal examination for impaction.
When no impaction was felt, the patient still wanted an enema
to relieve his symptoms. I then administered an enema because
I knew he would not be comfortable. There was no result from the
enema but at least he calmed down (Journal 101, pp. 21, 22). The
student identified the correct steps to solve the problem of this
patient and then with the assistance of the registered nurse (RN)
implemented the plan which relieved the discomfort of the patient.
Rose was able to connect what she had learned previously about
steps to take to lower a temperature and apply them to her patient:
There were two minor problems on my patient. He had an Aortic
Valve Replacement and was running a temperature of 100 degrees.
He felt warm to the touch. He was refusing to ambulate which is
a requirement post surgery. I knew that his temperature was probably
elevated because the room was so warm when I walked in. His respirations
were a bit fast probably compensating for his elevated temperature.
I also knew that I needed to get him to ambulate to help decrease
his temperature. I knew that I did not need to inform the nurse
unless the temperature was over 101 so I used what I had learned
previously. I rechecked his temperature and gave him a cool wash
cloth to cool him down and a towel to wipe his sweat. With these
small steps I was able to help lower his temperature with out
the use of medications (Journal 115, p. 22).
This is the last lab. There seems to be a feeling of relief in
the students tonight. It is a quiet evening for once because the
patient count is down. My activities are not as fast and furious
as they have been in the past few weeks. This quietness has given
the students time to think about what they are doing, and has
given me more time to observe more thoroughly and time to ask
questions of the students. I was able to visit the students sooner
and interact with them about the history of the patients they
had and what goals of care the students were planning for their
patients. The students seemed to have a good grasp as to what
was going on with the patients. Even when I asked them questions
about medications and treatment, they were able to answer my questions.
I did not see the confusion on their faces as they have had in
the past. The RNs had more time to spend in giving a report to
the students. This may have led the students to feel more comfortable
about their environment. Thus, they responded to me more easily.
The students also seemed more at ease with their problem-solving
ability. I am expecting them to function at this level by now.
Because it was quieter this evening, I was able to spend more
time with the students and their patients. For instance, Bill
had already done his assessment and was asking me about the edema
on the legs of the patient. He was saying that earlier that day,
according to the records, the edema was 4+ pitting. He felt that
it had gone down. But he was questioning whether the patient had
edema or was obese. Because I had time right then, we were able
to go in and assess the patient together. I was able to show him
the relationship of theory to the actual patient. I demonstrated
for the student how to check for edema. I verified his findings
and was able to show him other areas that needed to be evaluated.
I felt this opportunity to assess with the student was a good
way to help the student connect theory (assessment of the cardiac
conditions) with practice.
After the assessment, I was able to give suggestions to the students
about the care of a patient with dry, flaky skin on the legs.
At this point I was more in a telling mode and I really wished
I had spent time asking Bill questions as to how he would assist
the patient in the care of the skin. This may have increased this
student's problem-solving ability if I had taken the time to do
this.
I had the student apply lotion to the patient's flaky skin. I
felt this gave the student the opportunity to be with the patient
and learn about the patient. This patient was feeling better and
was bedridden and probably very lonely. She talked a long time.
By helping the student spend time with the patient, he did learn
about the psychosocial component of wholeness and made connections
in writing in his journal about the care of the patient. Bill
wrote: I felt I was able to help her a lot by talking with her.
She seemed very lonely (Journal 108, p. 9). Sometimes I wish students
could experience learning by osmosis from my brain so they could
learn about nursing faster and not miss the opportunities in caring
for the patient's real needs.
One of the goals for a student who had not been performing well
in the quarter was being met tonight. The student was keeping
me informed and problem solving on her own, which she had not
done in the past. This was real progress for the student. I assisted
the student in a new procedure. Since there was a time span between
when the procedure was taught and the performance of this procedure,
I reviewed the steps of the procedure with the student. She did
a good job performing the procedure. I felt she would be able
to do it again with minimal assistance. I could see on her face
the feeling of accomplishment.
Because it was a quiet evening and the students are more independent
at this point, I observed the activities of the students in their
ability to interact with patients, personnel, and each other.
People may have thought I was lazy or something just sitting there
at the nurses' desk, but it was like being a mouse in the corner
hearing and seeing what was transpiring. I observed three students
dialoguing with each other. This had not happened in the past
except for the very first day of lab. They were looking at each
other's materials and they were asking each other questions. Seeing
them collaborating with each other gave me a delightful, warm
feeling. The students looked more relaxed working together.
Post-conference is an important time to share information and
assist students in problem solving. I asked Bill to describe a
code that he had seen this evening. A code is when the patient's
heart or respiration has stopped and CPR was started. The description
he gave the group was quite thorough. He was able to answer the
students' questions and to clarify information without assistance
from me.
Linda had seen an endoscopy. She was also able to give a thorough
description, explaining exactly what she saw—the vocal cords,
the esophagus, the stomach, and the pylorus. It was fascinating
to hear her just rattle off the terminology and explain the anatomy
so well.
One of the students was concerned about seeing surgery the following
week. I suggested that she question some of the more experienced
students about surgery, so she could feel prepared to succeed.
She had genuine fear, but once she started talking with her peers
who had observed surgery her anxiety regarding an unfamiliar situation
was greatly reduced. This indicated to me that interaction with
other peers assist students in learning and decreases stress.
Problem Solving in Journal Writing
I incorporated the use of journals with the expectation that students
might become better problem solvers if required to respond to
specific questions about their nursing experience. I developed
a rubric with A part pertaining to problem solving and B part
pertaining to reflection. The following are the criteria used
for evaluating the responses:
1. Identifies one major significant problem.
2. Identifies a problem that arose.
3. Identifies one piece of knowledge needed to solve the problem.
4. Uses external resources when appropriate to solve the problem.
5. Identifies all logical steps as a part of implementation process.
6. Uses reliable external reasons to influence thinking.
7. Identifies one strength connect to patient care.
8. Identifies one weakness connected with patient care.
9. Names obvious thoughts and feelings connected to patient experience.
Each of these criterion was allocated 1 point each for a total
of 9 points. The mean was then calculated for the group. A simple
linear regression analysis was performed. There was no significant
change in the means (p>.05) across the 9 weeks (see Appendix
A6). Their problem solving skills remained consistent. In evaluating
how well the group answered the journal questions, percentages
of the answers to the questions were calculated (see Appendix
A6). The lowest percentage was question 3 at 78% and 5 at 79%.
When reviewing the students answers, the possible reasons for
these low percentages are that the students were having difficulty
in identifying the specific knowledge needed in problem solving,
and, therefore, they were unable to identify the correct logical
steps to take in the process.
Summary
These three "snap-shots" taken from the beginning, middle
and end of the quarter capture the progression of problem-solving
ability in this nursing clinical. At the beginning students lack
confidence in their ability and are very anxious. The last day
of clinical, everyone is more relaxed and they tend to meet the
challenges of nursing with greater ease.
Reflection
Refection is a process whereby a person revisits a lived experience.
There can be a sense of inner discomfort as the individual revisits
the experience. Removing the obstructing feelings is the beginning
of the reflective process. As a result of "mulling"
over this experience, the individual becomes open to new information
(Boud et al., 1985). This is when the individual reassesses prior
knowledge, feelings, and attitudes towards the problem and determines
the relationship of the old knowledge to make way for new information.
The person may choose to make a decision or postpone the decision
because of what has influenced the thinking. When the individual
reaches the "aha" experience, learning has taken place
and takes on a personal context (Boyd & Fales, 1983). Being
committed to action is the outcome of refection (Boud et al.,
1985).
The following was taken from Andrea's journal: A problem arose
not with my patient but my patient's roommate. The roommate was
in restraints and he was very confused. Every time I was in the
room, he wanted my help or wanted to talk to me. He kept telling
me that he was feeling very closed in and needed the restraints
off. I wanted to help him. The whole time I was there I do not
believe anyone helped this man. I knew that a patient in restraints
needed to be checked more often, and just because he was confused,
I felt he needed someone to talk to him and help orientate him.
I tried to get help from the nurse, but she was busy with an admission
and another patient who was in great pain. I knew the patient
needed the restraints but he needed his other needs addressed.
The patient's discomfort and distress was what influenced my thinking.
He kept calling out and talking out-loud when I was in with my
patient. I talked with the registered nurse, and she helped me
understand the patient but nothing was done. Finally around 5:30,
I found the CNA who came in to talk to the patient and assist
him to the bathroom. The problem was solved by the CNA taking
him to the bathroom and allowing him to sit up in bed. The lights
were turned on, and his mind was put at ease (Journal 101, pp.
2, 3).
Because of the inner sense of discomfort (conflict) within the
mind and knowledge that had been taught to her from Nursing 1,
the student was able to solve the problem. When we talked about
the experience in post-conference, she was determined not to let
this happen to any of her patients whom she would care for. This
statement by her was an outcome of reflection. I feel that if
she would encounter any patient with this kind of problem again
she would act upon the problem based on the previous reflection.
Reflection is considered a process and can be intentionally taught
(Boyd & Fales, 1983). As an educator, I assigned each student
to write in a journal answering specific questions. Following
are the questions (see chapter 3 for reasons for questions and
explanation for reflective score) answered by the students in
their journals and the criteria and in brackets stages of reflection
for questions 1, 2, 3, 4, 6, 8, and 9.
1. Looking back, do you think the problems that you identified
were the most important ones for the patient? What additional
problems do you now identify as the result of caring for the patients?
Criteria: Identifies other related problems which may include
reasons for the problem. (Integration)
2. Identify a problem or a need that arose during the shift. Explain
the circumstance of this problem including whom, what, when, where,
and how urgent was the problem?
Criteria: Explains reason for urgency or lack of urgency. (Integration)
3. What knowledge was required for you to solve the problem?
Criteria: Identifies connecting piece of information needed. (Association)
4. What resources helped you to solve the problem?
Criteria: Recognizes personal resources as a resource. (Association)
5. What steps did you take to help solve the problem?
6. What influenced your thinking about this problem?
Criteria: Uses internal reason to influence thinking. (Association)
7. What were your strengths for this clinical experience?
8. What were your weaknesses and tell how you will strengthen
these weaknesses the next clinical experience?
Criteria: Explains how to improve on his or her weakness. (Validation)
9. What were other thoughts and feelings about your clinical experience
today?
Criteria: Expands reason for thoughts or feelings from the experience.
(Attendance to feelings and Validation)
In order to determine the presence of reflection, I developed
a rubric (see Appendix A4 and chapter 3) that assessed the reflective
elements by the questions that were asked. The students responded
to 9 questions. Seven questions were given a reflective score
of 1 point each, making a total possible reflective score of 7
points. Each student was given a reflective score based on the
analysis of answers to the questions. The mean was calculated
for the 19 students for each week during the clinical experience
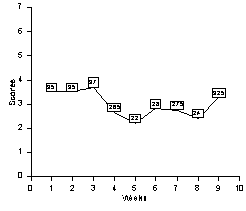
(see Figure 1 and Appendix A5). A simple linear regression analysis
for change was performed. There was no significant change in the
means (p>.05) across the nine weeks (see Appendix A7).
To assist in understanding which questions the students may have
had difficulty in reflecting upon, the percentages of each B criteria
for the 19 students were calculated. For the first week, the percentage
answered for each reflective element (see Appendix A7) was: question
1 at 56%, question 2 at 50%, question 3 at 31%, question 4 at
19%, questions 6 at 44%; question 8 at 69%; and question 9 at
53%. By week 5 (the lowest

Figure 1. Mean weekly reflective score of unpaired students over 9 weeks.
group mean reflective score) the percentage answered was: question
1 at 50%, question 2 at 29%, question 3 at 07%, question 4 at
21%, question 6 at 14%, question 8 at 71%, and question 9 at 50%
answering the questions reflectively. The questions that seemed
to have the greater amount of change downward were questions 3
and 6. Questions 1 and 8 had the highest percentage. Calculation
of the average of the percentages for the nine weeks revealed
that question 3 at 21%, question 4 at 25 % and questions 6 at
35% were the lowest for the quarter. These results may indicate
that students have difficulty in connecting knowledge needed in
solving problems, that they do not recognize themselves as a source
of knowledge, and do not always know what influences their problem-solving
decisions. This would be consistent with Baxter Magolda's (1992)
findings on reasoning and knowing in college students.
A possible reason for reflection not increasing to a higher level
than the beginning score may be that students did not journal
conscientiously because they felt they did not have time or interest
in writing in their journal. One student commented, You must know
when we are writing well and when we are not. She pointed to her
journal and asked me to look at it. As I did, she remarked, Now,
can't you see I did not do a very good job last time? She then
stated to me that she would try to do better in the future.
A possible second reason may be because I chose not to give extensive
feedback in the journals. I wanted to remove my influence in the
reflective process for both the unpaired and paired students.
In Lewinian's (cited in Kolb, 1984) Model of Experiential Learning
in order for students to move from the observation and reflection
level to the formation of abstract concepts and generalizations,
they need immediate feedback. Lack of improvement in reflection
may not have taken place since feedback was infrequent.
Themes
The themes emerged from the written journals and personal notes
for this case study. The themes include emotions, ways of knowing,
collaboration and dialogue, communication, learning, connecting
theory with practice, and professional role.
Emotions
As a part of the learning process and critical thinking, emotions
can motivate or inhibit what is being learned and what is being
reflected upon. "Good moods, while they last, enhance the
ability to think flexibly and with more complexity, thus making
it easier to find solutions to problems, whether intellectual
or interpersonal" (Goleman, 1994, p. 85). In the journal
writing the students freely expressed their feelings.
Positive emotions motivated the student to continue in the clinical
experience. It gave them a relaxed warm feeling, making the day
a worthwhile experience. Positive emotions made the student willing
to come back again and learn in the clinical setting. Positive
feelings were expressed in statements such as: I was inspired
by the hope and tenacity of my patient (Journal 109, p. 15). I
enjoyed my clinical experience. I feel that when I am at my clinicals
that I learn the most about nursing (Journal 110, p. 4). Feelings
of affirmation: The nurse told me that she was glad that I was
there this evening (Journal 115, p. 3). Often these positive feelings
were expressed in post- conference when the students were discussing
the events of the day. I could almost see the positive feelings
in the students' faces and hear it in their voices.
These positive feelings promoted self-esteem: This lab helped
me to bring up my confidence level from last time. And I also
felt I got a lot accomplished with the help of the rest of the
health care team (Journal 112, p.11).
Negative feelings bring the opposite effect to the student. Negative
feelings can be barriers to reflection (Boud & Walker, 1993).
"Being in a foul mood biases memory in a negative direction,
making us more likely to contract into a fearful, overly cautious
decision. Emotions out of control impede the intellect" (Goleman,
1994, p. 86). Because an individual is in a foul mood, this mood
can effect self-esteem and the confidence to make a correct decision.
Although anxiety can promote a state of alertness, it often brings
the feelings of disorientation, confusion, and discouragement
(Alfaro-Lefevre, 1995). Negative feelings such as: I was feeling
really overwhelmed before lab. I came a little too close to using
this lab as my drop lab. Just the psychological impact of having
two patients really affected me (Journal 108, p. 3). When I started
my patient care today, I was a little bit nervous. I did not want
to make the same mistake that I made last time (Journal 112, p.
8). I felt disorganized and a little disoriented before change
of shift for p.m. shift. Two patients add a lot of paper work
I was not used to (Journal 106, p. 4).
The feeling of anxiety coupled with expectations of how the student
should perform affects how the student performs throughout the
clinical day. I was not aware of my patient's post-operative status.
I was unprepared and the nurses were too busy to help so I had
an anxiety attack. Terrible!!! I allowed my anxiety to influence
my whole night and all following procedures. It exhausted me to
be so emotional, and I consequently became very disorganized.
This can be dangerous as a nurse and is unprofessional (Journal
117, pp. 12, 13). The negative feeling of anxiety led to decrease
in confidence in her abilities to think through the problem. Fortunately
for her, the nurse and I influenced her thinking so that she could
calm down and function the rest of the evening.
Ways of Knowing
There are many ways of knowing. All of them are important in problem
solving and critical thinking. One of the ways of knowing is knowing/caring
for the patient (Jenks, 1993). When a student gets to "know"
his or her own patient, the student can converse and intervene
more readily in the care of the patient.
Crystal felt knowing the patient was her strength. My strength
this evening was knowing the patient's history. It helped me to
understand any other problems they might be going through (Journal
105, p. 14).
Getting to know the patient and spending time communicating help
patients to relax. I needed patience with J. D. He could be very
demanding at times, but when I could talk to him calmly and take
time to listen to him. I think it made him relax (Journal 101,
p. 23).
Students felt that they were able to get acquainted with the patients
even if it was for a short period of time. Although I was only
with my patient for three hours, I felt I was able to get to know
him better (Journal 112, p. 12).
A second way of knowing is the use of previous knowledge. Without
a "base" knowledge of some kind, students cannot problem
solve or even learn. "One of the most important principles
of educational psychology is that the most important single factor
that influences learning is what the learner already knows"
(All & Havens, 1997, p. 1218). Cholowski and Chan (1995) in
describing the "Knowledge Driven Model" of problem solving,
concluded the more existing knowledge the student has, the better
he or she can integrate the clinical data in making appropriate
clinical decisions. Although I had specifically asked what knowledge
was brought to the problem-solving process, the responses to this
question can be divided into three areas:
1. Information the students learned from Nursing I and II and
from the sciences: Knowledge to check intake and output [from
Nursing 1] (Journal 106, p. 2). Knowledge that was required was
the fact that I knew diversion is a good way to help with pain
[Nursing II] and also the knowledge of helping to reduce anxiety
by giving the patient reassuring statements of help calm the patient
[Psychology and Nursing II] (Journal 102, p. 5). I needed the
knowledge of the function of the bowels to solve the problem [anatomy]
(Journal 101, p. 2).
2. Knowledge the students learned this quarter (Nursing III):
Third quarter nursing knowledge (Journal 119, p. 5); I had to
know that the I.V. sites should not leak fluid or blood, and when
they are puffy or swollen, this is not normal. The I.V. solution
could be leaking into subcutaneous tissue and the needle dislodged
from the vein (Journal 101, p. 13).
One of the "problems" I had was that I thought I had
heard a murmur. I heard it over the right second/third intercostal
space. The S2 was stronger than the S1 and I heard a sh—sound
similar to the one I had heard in the cardiac assessment video
(Journal 112, p. 16). The student is comparing the sound that
she heard in the patient to what she had heard from a video that
was required for class that week.
3. Common sense: Common sense basically helped me to identify
the problem (Journal 119, p. 1). I think that with these problems
it was mainly common sense I used to solve the problems (Journal
114, p. 2).
Knowledge was an important factor in influencing the students'
thinking. Determining what influences your thinking is important
in problem solving. The techniques we learned about communication
in Nursing Fundamentals and Nursing 154 is what influenced my
thinking (Journal 102, p. 9). My thinking was influenced by what
I had learned from class with patients with elevated temperatures
(Journal 105, p. 19).
Collaboration and Dialogue
Dialogue is important in making learning an active process (Lambright,
1995). Being able to feel comfortable as a part of the team and
a nurse interested enough to dialogue with the student made the
student feel important and needed. I had a nurse who expected
a lot from me—which was good for me. He had time to explain
and help me. Other nurses can be too busy sometimes. I was happy
that he wanted to help me take out a JP drain. I liked it when
nurses were willing to let me help even if it was not my patient
(Journal 101, p. 24).
It can be detrimental to the student if she feels like she cannot
communicate with the nurse. I need more confidence when communicating
with the others nurses. I tended to just listen, [not] sharing
my thoughts and feelings. When it is time to give report at night,
I tend to freeze and forget the important things to mention to
the nurse (Journal 101, p. 23).
Communication
One of the questions the students answered was: What are your
strengths? The most repeated strength was communication, especially
with the patient. "Critical thinkers are good communicators,
realizing that mutual exchange of ideas is essential to understanding
the facts and finding the best solutions" (Alfaro-Lefevre,
1995, p. 10). It was important for the student to use communication
in getting to know the patient. I felt like I had good communication
skills with my client. I obtained the information I needed in
a way that did not threaten or belittle my patient (Journal 110,
p. 4).
Marie felt that communication with the nurse helped in solving
the problem. My strengths for this clinical experience were 1.
Good communication with nurse, 2. Good communication with patient,
and 3. Good communication with patient's family. When a problem
arose, I would inform the nurse and try to solve the problem by
the end of my shift (Journal 112, p. 2).
Learning
It may seem unconventional to have learning as a theme, but the
words I learned a lot in clinical today were expressed in most
of the journals. According to Kolb (1984), "learning is the
process whereby knowledge is created through the transformation
of experience" (p. 38). As the result of reflecting on the
clinical experience, student learning took place. Because of the
perceived learning process, knowledge is created and recreated
in the minds of the learner (Kolb, 1984). Learning in an experiential
climate like the clinical setting "involves the whole learner
in cognitive, psychomotor and affective aspects of the learning
event" (Reilly & Ommerman, 1992, p. 165). For the students,
the psychomotor domain was often identified in the procedures
that they participated in and what they perceived as learning.
They believed they learned by "doing": This clinical
session was a great learning session. I was able to observe the
nurse pull the sheath of a patient who was post angiogram test
[a test to view the coronary arteries of the heart]. I got to
take vitals during the procedure (Journal 118, p. 3).
I feel that I really took some steps in this clinical in applying
theory to practice. I got to perform procedures such as injection
and giving a bath. I was surprised at how sure I was when I helped
the nurse change an occupied bed. I had organized everything we
needed and was quite confident and even took charge (Journal 117,
p. 11).
An example of learning in the cognitive domain was: I really loved
this clinical experience. I learned a lot about the monitors and
found that I remembered what I had learned in first and second
quarters (Journal 109, p. 2).
An example of learning in the affective domain was: I learned
a lot about care of the patient post cardiac surgery. I also found
out how it would affect me if a patient died. I did not know if
I could handle that part of nursing. Now I know I can get through
it (Journal 109, p. 7).
These learning experiences portrayed an eagerness to be in the
clinical setting because the students felt they learned a lot.
The day may have started out as anxiety producing but ended up
as a gratifying experience. Bill was overwhelmed in ICU (Intensive
Care Unit). He felt out of his element. Because the nurse assisted
him in learning, it ended up being fun, I learned a lot and feel
more confident (Journal 108, p. 5). I believe that these learning
experiences are what motivated the students to learn more and
to come back to the clinical setting. I had a great clinical experience
last night, and it is not only challenging but fun. I think I
am actually beginning to look forward to clinicals rather than
being afraid of them. A lot of what I have learned this quarter
and past quarters is beginning to make sense (Journal 102, p.
13).
Connecting Theory With Practice
One of the reasons for having students reflect is to provide the
opportunity to assist the student in connecting theory with practice.
The clinical setting is the place where students can apply theory
to real clients and real problems (Reilly & Ommerman, 1992).
Through exposure to real-life situations the students were able
to grasp the concept of caring for the individual's whole being.
The students integrated the concept of spiritual care: I appreciate
that we talked about the power of prayer in post conference. I
truly believe in the power of prayer as mentioned. There are many
things you can do with patients if you do not feel comfortable
about praying with them, such as listening while they pray. Last
night I told my patient that I would remember her in my prayers
before I went to bed. I guess a small gesture like that is also
therapeutic for the patient as well as myself (Journal 111, p.
8).
The students also applied concepts of trust and compassion: It
is a shame how some patients can feel lonely and neglected because
the nurses or CNAs are way too busy dealing with more than two
patients at a time. I think that to be able to spare more than
a few minutes to sit and just talk to my patient felt really good.
I was able to grasp the concept of compassion and trust with my
patient (Journal 115, p. 19).
Students learned about culture in the care of their patient: The
patient could only speak Spanish. If the patient does not understand
his treatment or the rationales behind them, he may not cooperate
to the fullest extent, thereby putting him at risk for possible
non-compliance. Beside the inability to communicate, the Hispanic
culture, I believe, has a need for a man to be very independent
and self-reliant. This factor may play a major role in the future
outcome of this patient's well-being. I used a CNA to interpret
for me, but I wonder if they were understanding me. This experience
really taught me a lot about how cultural beliefs are a big part
of nursing and a patient's well-being (Journal 102, p. 17).
Giving the reason for treatments to a patient with respiratory
problems relieves anxiety and the feeling of helplessness. I found
the patient close to tears when I entered the room. Upon investigating,
I discovered that he wanted his tracheostomy tube out. I explained
to him the reason he had the tracheostomy was to ensure that he
could breathe on his own, working towards strengthening his respiratory
muscle so that they eventually could take the tracheostomy tube
out. I think that this really helped him feel better (Journal
118, p. 10).
Professional Role
The clinical experience provides an avenue through which the student
becomes socialized into the profession, its values, and accepts
professional responsibility (Reilly & Ommerman, 1992). Some
of the students were able to acquire an understanding of the role
and responsibilities of the nurse as a result of participating
in and reflecting about the hospital setting.
Becoming a nurse: I am struggling with self-confidence. I can
see myself growing, though, and with each clinical experience
I find myself falling more and more into the role of the nurse,
not Joan only, but Joan as a nurse, and I really am starting to
believe I am capable of this (Journal 102, p. 13).
Role modeling: I thought how nice certain nurses are and how I
would like to be nice too (Journal 106, p. 11).
Meeting the goals of what the student perceives a nurse doing
is exemplified in: I went into nursing wanting to help people,
and I feel that I really try to do this. People really appreciate
it (Journal 110, p. 113). I cannot wait to move up and be more
of a leader in my field. Successful knowledge is so important.
It is the key into being the kind of person I want to be! (Journal
119, p. 7).
Summary
In this chapter, I told the stories of nursing students as they
learn to problem solve and care for patients in the hospital setting.
Journal writing was the method used to assist students to think
about their clinical experience. The students gave their perspective
of the problems they encountered and the factors that affected
them. The themes that emerged from the students' journals were
emotions, knowing the patient, collaboration and dialogue, communication,
learning, connecting theory with practice, and professional role.
The analysis of the journals by the reflective rubric showed that
the reflective process remained consistent during the nine weeks.
The following chapter shares the lived experience of paired nursing
students as they worked and journaled together in the clinical
setting. The results from the rubric analysis of the paired nursing
students' journal will be explained.